Today I would like to talk about my ACME project details and its format. The Advance Course in Medical Education(ACME) is a project-based course of 6-month duration and has two contact sessions of 5 days and 3 days with one overlapping day when two batches meet and interact as per NMC.
Title: Introduction of objective structured clinical examination as an assessment tool for undergraduate students in Community Medicine

What is ACME?
Before we talk about my ACME project let me introduce what is ACME, and why it was introduced by the erstwhile MCI.
Eligibility For ACME
In 2014, India introduced the Advance Course in Medical Education (ACME) as part of a multi-tiered approach to enhance the quality of medical education.
ACME is a 6-month project-based course comprising four phases, including two onsite phases and two phases of online learning modules.
The program is intended for 30% of faculty in medical institutes, covering various specialties.
Faculty members should full-time be working with the institute and have completed RBCW or BCME to be eligible to apply for ACME.
At least three years of teaching experience.
Nomination will be sent by the institute to their respective nodal center with a dually filled application form along with the course fee DD(15000 INR).
Enrollment and conduct of the program are governed by established rules and norms, and eight batches of approximately 1200 college faculty members have completed the course.
| Batch A | Batch A | Batch A |
| 5 days onsite | 6 months online for discussion on 4 educational themes. Also, have some content delivered electronically. Project work | 3 days onsite Present their project Encourage networking and mentoring partnerships Batch B 5 days onsite |
Introduction/ Background ACME:
It is said that the Indian Medical Graduate (IMG) is not competent enough to serve at the PHC of the village. The fault also lies with the present medical teaching methods where we don’t teach a basic concept of primary health care the way they are going to be applied in the field. For example preparing ORS, epidemic investigation, chlorination of water, and many more are taught in the classroom of Community Medicine. If it is implemented in the form of the objective structured case examination (OSCE) then the teacher and students have to teach and learn in that manner and so it will overcome gaps in the essential knowledge for those skills. (1–3)
It has been observed that the traditional way of assessing students does not include the affective and psychomotor domain assessment most of the time, so the introduction of a structured way of assessment like OSPE and OSCE in the subjects will not only assess the student for the higher domain but also provide feedback to the teacher and student for the scope of improvement.(1,4–6)
Department of Community Medicine have been assessing students for various skill like chlorination of water ORS preparation and counseling in oral viva voce and spotting which in is not a structured way of assessment as emphasized in Competency-Based Medical education (CBME) and mostly testing the knowledge of the students. So with the idea of implementing the OSCE in community medicine, this study has been undertaken with the objective of introducing OSCE as an assessment tool for community medicine and improving the understanding and skills of undergraduates for various public measures.
Literature Review For ACME:
Many have documented the superiority of OSCE over the traditional way of assessing in many subjects like physiology, Biochemistry Anatomy, and Community Medicine. (4,5,7,8)
OSCE: The objective structured clinical examination (OSCE) is a method of objectively testing the clinical and practical knowledge and skills acquired during the medical curriculum.(9)
Following are the steps which can be used for designing OSCE.(2,3)
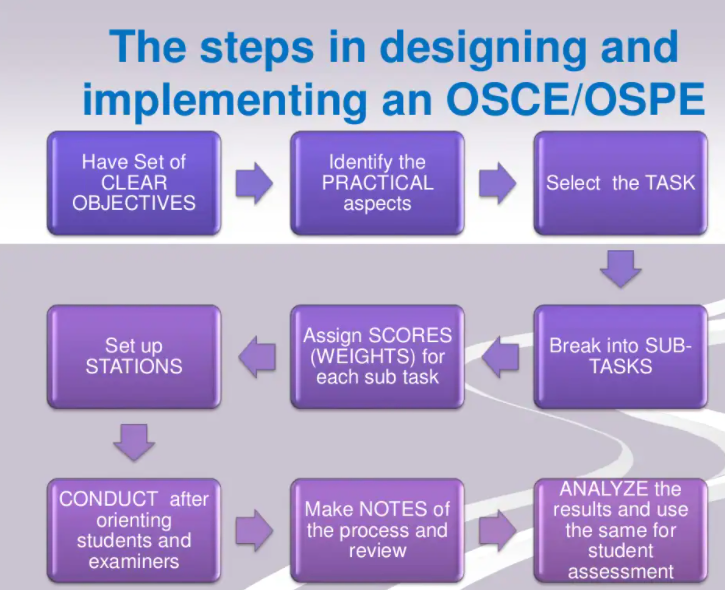
In PSM, students are usually not asked to perform a particular practical related to public health, it is mostly covered in viva or theory which is again based on overall performance rather than the candidate’s individual practical/counseling skills. Hence, individual competencies might not be tested. Due to this, students do not bother much about exact procedures while performing a skill. They are vague in answering questions, lacking focus, and objectivity.(5)
Aim of ACME Project:
Aim: to improve the public health-related skills of undergraduate students.
Objective/s:
1. To introduce the OSCE assessment tool for community medicine
2. To know the perceptions of teachers and students regarding OSCE as a tool for assessment
3. To document if the OSCE helps in improving the skills of the students
Material & Methods:
Study settings: Second-year MBBS students of Govt Medical College Surat.
Study Duration: from April 2022 to Sept 2022.
Study design: Mixed method study design. There will be an educational intervention study followed by a focal group discussion (FGD) of students and teachers for the OSCE in community medicine.
Study methodology:
All the faculties and residents involved in the study will be trained for uniformity in assessment using OSCE stations. Pre validated OSCE checklist will be used for assessment and the effectiveness of OSCE will be assessed through a student’s and teacher’s feedback questionnaire that will be prepared after the literature search and validation by the faculty in Community Medicine and medical education. The questions administered will be checked for the coefficient of reliability by Cronbach’s alpha. The students will be sensitized and oriented toward OSCE beforehand by explaining the OSCE pattern and discussing sample questions during their practical classes. Exact details and the timing for the station will be chalked out for the study based on piloting.
After informing students regarding their voluntary participation they will be enrolled in the study.
Sample size: 250 students from the second year (2020 admission batch)will be enrolled after being informed consent. There will be a posting of 40 students in each batch for four weeks. So following OSCE station will be exposed to the batch of 35 to 40 batch of students.
Sampling technique: purposive sampling method, all the students who are willing to participate will be taken from the 2020 admission batch.
FLOW-CHART OF ACME STUDY
1. A total of 10 competencies were chosen from the NMC curriculum document for Community Medicine where the level of learning is expected to be shown how and are taught in clinical postings in second year MBBS.
2. Faculties dept. of community, medicine will be briefed about the concept of OSCE with the help of a PowerPoint presentation. They were invited to participate in the study and development of the OSCE station.
3. Selection and Improvement of 10 OSCE checklists after receiving of feedback for the same from faculties and experts. Decision on time and marks of each station. OSCE checklist will be uploaded to the App platform for data collection
4. Ten stations will be finalized after the presentation/discussion with teachers. Each batch will be exposed to five stations out of 10. The duration for each station will be 10 min. there will be a resting station between the actual stations. Teachers/senior residents acting as an examiner will be using Appsheet note performance of students.
5. Actual examination will be conducted with prior information to the students. Consent will be taken and the students will be assured that the marks secured in this examination will not be counted for the final assessment. The team will be Associate and Assistant Professors, tutors, and resident doctors from the dept. of Community Medicine
6. The perceptions of teachers and students will be collected using Google forms which include some statements. Likert’s scale will be used to know their degree of agreement with the statement. Immediate feedback regarding performance will be given to students. FGD will be conducted later to interact with faculties and students to know more about their views on OSCE
7. Comparing their performance with routine Conventional practical examination (CPE) Data analysis and reporting.
The following OSCE stations will be used for the study.

In the second stage of the study, all the faculties and the sample of the student will be arranged for focal group discussion for getting qualitative data on the new assessment tool OSCE.
FGD: the objective of FGD for this study is to know the understanding of the students and teachers about the newer approach to learning. The following key question will be added to know about their view on OSCE.
1. What is your view/opinion on OSCE station in CM
2. How it is helpful in learning important concepts in CM
3. Why should stick to the traditional approach or OSCE?
There will be 3 to 4 FGDs for students and 2 for teachers which will saturate the objective of the FGD. Content analysis will be done and findings will be helpful for the improvement of teaching-learning in community medicine subject.
Validation of questionnaires/checklist: pre-validated feedback/perception scale will be used from the literature.
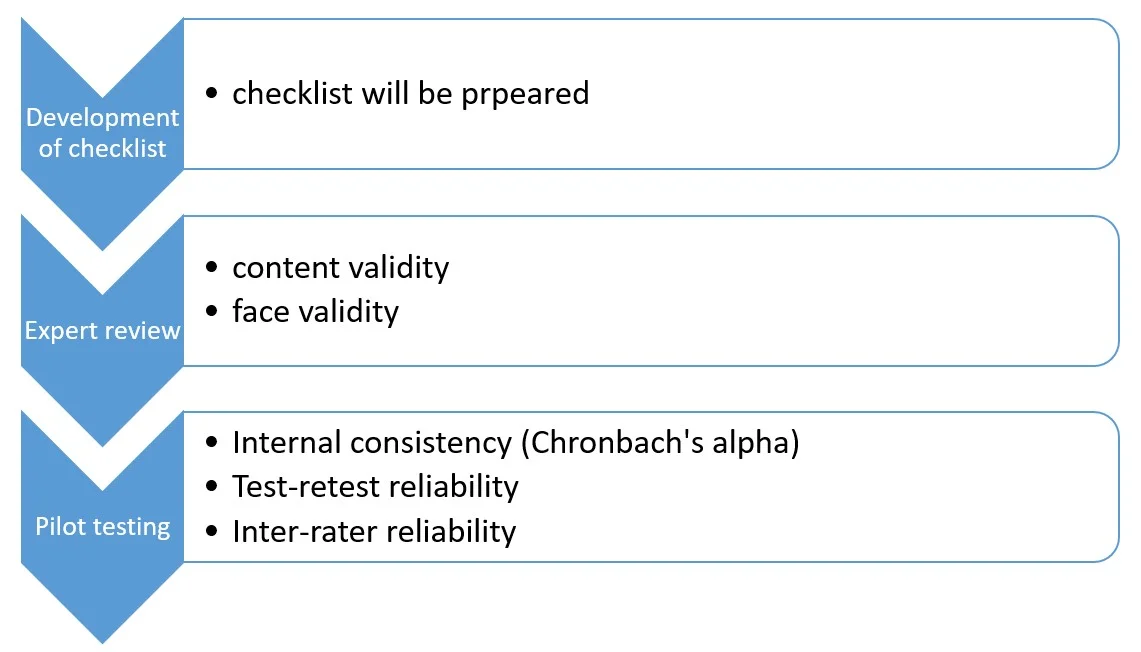

Inclusion & Exclusion criteria:
Second MBBS students who are willing to participate will be included and the rest will be excluded.
Statistical analytical approach
Data entry and analysis:
Results of external validation will be presented and the co-efficient of reliability Cronbach’s alpha will be calculated
Data will be collected using a mobile-based App customized for the purpose.
Data will be entered in excel and analyzed using SPSS.
Descriptive analysis:
The total score per participant for OSCEchecklist will be calculated and presented as percentages, mean, and standard deviation.
Inferential statistics:
As the assessment drives learning there should be greater learning in skills/topics assessed by OSCE.
All the students are exposed to OSCE during their clinical posting. The effect of OSCE will be compared with the results of the conventional practical examination (CPE) of the same batch during their end of posting using structured viva-voce and MCQs.
CPE will be 20 marks 2 marks each from 10 stations similarly 10 marks viva: 1 question from each station.
The mean scores of the topics assessed by the OSCE and the mean scores of the topic not assessed by OSCE will be compared using the student’s t-test.
Table: Score obtained during the end of clinical posting assessment (MCQ &Structured Viva)
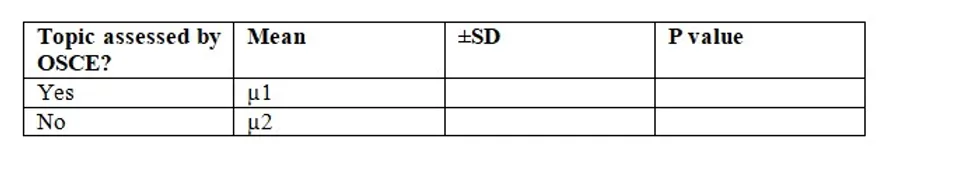
The theme will be derived from the FGD using content analysis for their perception of OSCE.
References (Vancouver referencing style):
1. Abraham RR, Raghavendra R, Surekha K, Asha K. A trial of the objective structured practical examination in physiology at Melaka Manipal Medical College, India. Adv Physiol Educ. 2009;33:21–3.
2. Scott D, Jenkinson A. How to OSPE.
3. Dinesh T. medical-education-technologies-ospe-osce [Internet]. Web presented at; Available from: https://www.slideshare.net/dineshthangavel1/medical-education-technologies-ospe-osce
4. Rajani M, Ghewade B. Comparison of student performance by assessment through Objective Structured Practical Examination versus the Conventional Method for second year MBBS students in Microbiology. J Adv Med Educ Prof. 2020;8(3):121–6.
5. Shenwai M, Mardikar P, Joshi N, Joshi R. Introducing objective structured practical examination as a formative assessment tool for phase I medical professionals in physiology. Natl J Physiol Pharm Pharmacol. 2020;10(8):1.
6. OSCE MANUAL 2014 Objective Structured Clinical Examination الهيئة السعودية للتخصصات الصحية Saudi Commission for Health Specialties.
7. Mard SA, Ghafouri S. Objective structured practical examination in experimental physiology increased satisfaction of medical students. Adv Med Educ Pract. 2020;11:651–9.
8. Jena M, Bhat V, Indrani K. Relevance of Objective Structured Practical Examination Reinforced with Multiple Choice Questions as a Tool of Learning and Retention of Knowledge in Pathology among the Undergraduate Students. J Med Sci Health. 2015 Jun;01(02):30–3.
9. Carolin A, Devi PTV. Objective structured practical examination as a formative assessment tool compared to the traditional method for third-year M.B.B.S. community medicine students. Int J Community Med Public Health. 2019 Sep;6(10):4285.
Outcome Matrix:
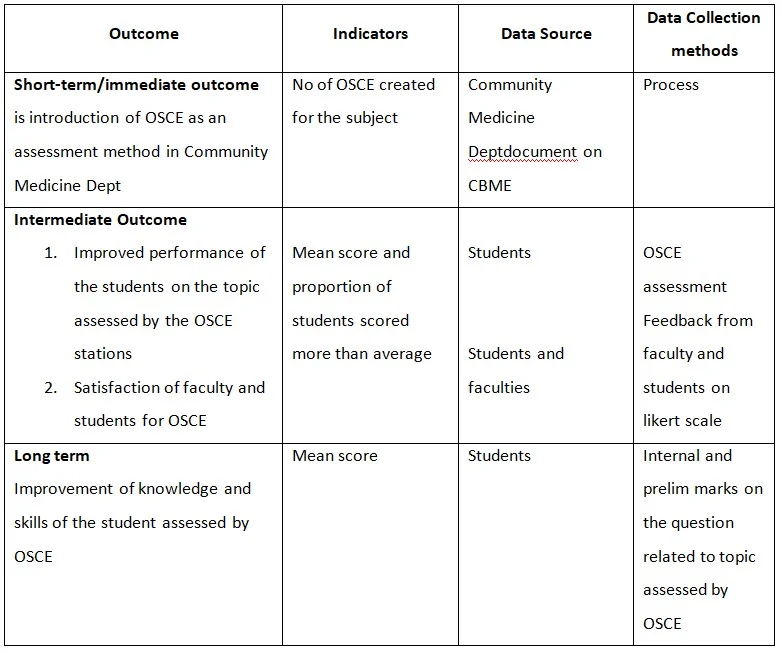
Gantt Chart:

Concept Mapping:


Add a Comment
You must be logged in to post a comment