Explore the intersection of risk factors and health in the modern era. This comprehensive guide, “Risk Factors Demystified: Decoding Risks and Health in the Contemporary World,” delves into the various factors that impact our well-being. Discover how understanding and managing these risks can lead to a healthier and more informed life.
GIS Demystified! Your Comprehensive Guide to Geospatial Technology
Explore the world of Geospatial Technology with our comprehensive guide on GIS Demystified. Discover how geospatial data, mapping, and analysis work together to provide insights for diverse industries. Dive into this informative article to gain expertise and insights on geospatial technology.
Shining a Light on the Dark Side of Radiation: The Hidden Hazards You Need to Know
From the dangers of radon in our homes to the risks of nuclear accidents, we will shine a light on the dark side of radiation to protect ourselves.
Disease Prevention: Levels of Disease Prevention in 2023
In this article, we’ll discuss the three levels of disease prevention in 2023 and how to best utilize them. We’ll also go over the benefits of each level.
What is Ergonomics? Ergonomics In The Workplace All You Need To Know
Ergonomics is the study of how people interact with their environment, particularly in the context of work.
Probability in Statistics: Types of Probability Distributions Examples and Characteristics
In probability and statistics, a distribution is a function that describes the likelihood of different outcomes in a random event. Simply, it is a frequency plotted as a graph or shown as a table.
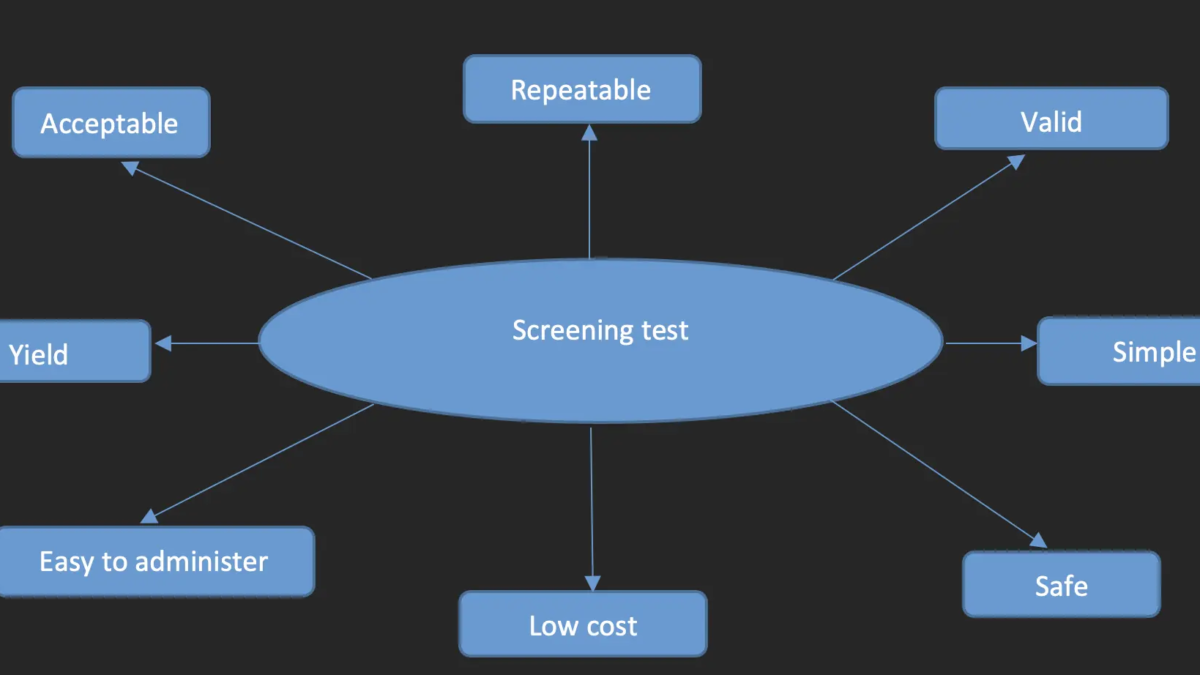
Screening Test: Types Uses Validity And Evaluation
The search for unrecognized disease or defect by means of rapidly applied tests, examinations, or other procedures in an apparently healthy individual is known as screening.
Descriptive Statistics & Inferential Statistics: How to Answer to Statistical Exercise in five Steps
In this article, we will discuss how to attempt such a statistical exercise in simple easy steps and answer it correctly.
What is Epidemiology?
Policymakers use this information to formulate rules, regulations, and guidelines for the prevention and control of the disease. The role of an epidemiologist is like a detective who tries to solve the puzzle of cause and effect. Which ultimately helps in restoring public health.
Epidemiology- What is Incidence and Prevalence in Epidemiology? Incidence Vs Prevalence
Is it possible to have a disease where the incidence rate is going down but the prevalence rate is going up?